$48.5
Million
Truck Accident Case
We took more than 60 depositions in five different states. Because of Stephenson’s tireless advocacy, shortly before the trial was to commence, the defendants settled the case for $48.5 million.
Superbugs in the Elderly

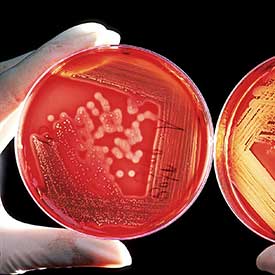
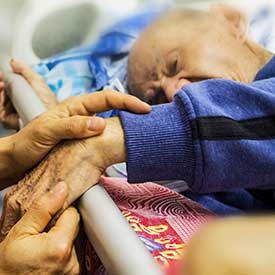
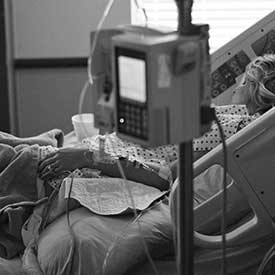
In September, the Centers for Disease Control (CDC) released a worrying report about three superbugs, germs that are resistant to antibiotics. They described the situation as “urgent.” Two of the three microorganisms are especially prevalent in medical settings and nursing homes, adding to the vulnerability of elderly people or those who are already sick.
The superbugs of concern for nursing home residents are Carbapenem-resistant Enterobacteriaceae (CRE) and Clostridium difficile. Dr. Tom Frieden, Director of the CDC, said, “CRE are nightmare bacteria. Our strongest antibiotics don’t work and patients are left with potentially untreatable infections.” CRE kills up to half of the patients who get bloodstream infections from the disease. Clostridium difficile, or C diff, is a serious diarrheal infection usually associated with antibiotic use. It causes about 337,000 hospitalizations and at least 14,000 deaths every year in the United States, according to CDC data.
A study published in the April 2013 issue of Infection Control and Hospital Epidemiology found that long-term care facility residents are eight times more likely to contract a particular strain of E. coli. This finding demonstrates the need for long-term care facilities to improve their current practice of antibiotic use and to institute infection controls.
The U.S. Department of Health and Human Services estimated in a report to Congress that by the year 2050 there would be 27 million people in the U.S. in long-term care. Thus, the dangers posed by these superbugs are appropriately described as urgent.
As a personal injury attorney, I urge everyone who has a loved one in an Indiana nursing home to question the facility’s medical providers about how they are avoiding overuse of antibiotics. Long-term care homes must practice good antibiotic stewardship, ensuring that our seniors are not endangered by unnecessary or poorly monitored antibiotic use.




 Mike Stephenson has 40 years of experience and is a trusted advisor to many individuals and companies. His current practice is dominated by civil litigation in state and federal courts. He focuses much of his time on handling catastrophic injuries caused by all types of accidents, including motor vehicle, trucking, workplace injuries, product liability, and fire, just to name a few. He also works extensively in construction accidents. [
Mike Stephenson has 40 years of experience and is a trusted advisor to many individuals and companies. His current practice is dominated by civil litigation in state and federal courts. He focuses much of his time on handling catastrophic injuries caused by all types of accidents, including motor vehicle, trucking, workplace injuries, product liability, and fire, just to name a few. He also works extensively in construction accidents. [ 


